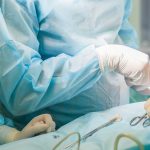
After a near-fatal crash unveiled a massive cancer in his throat, Dan Kenney turned to a groundbreaking clinical trial led by Gregory W. Randolph, MD, FACS, FACE, to avoid disaster for a second time.

Dan Kenney held on to the steering wheel for dear life.
The breaks to his garbage truck had failed midway down a hill on his regular trash route through Amesbury. His vehicle was hurtling toward a home at the hill’s base, leaving him to make a split-second decision: either turn left into trees and a lake, or cut the wheel in the opposite direction. Dan turned the wheel as far right as it could go, and the truck flipped over onto the side of the road.

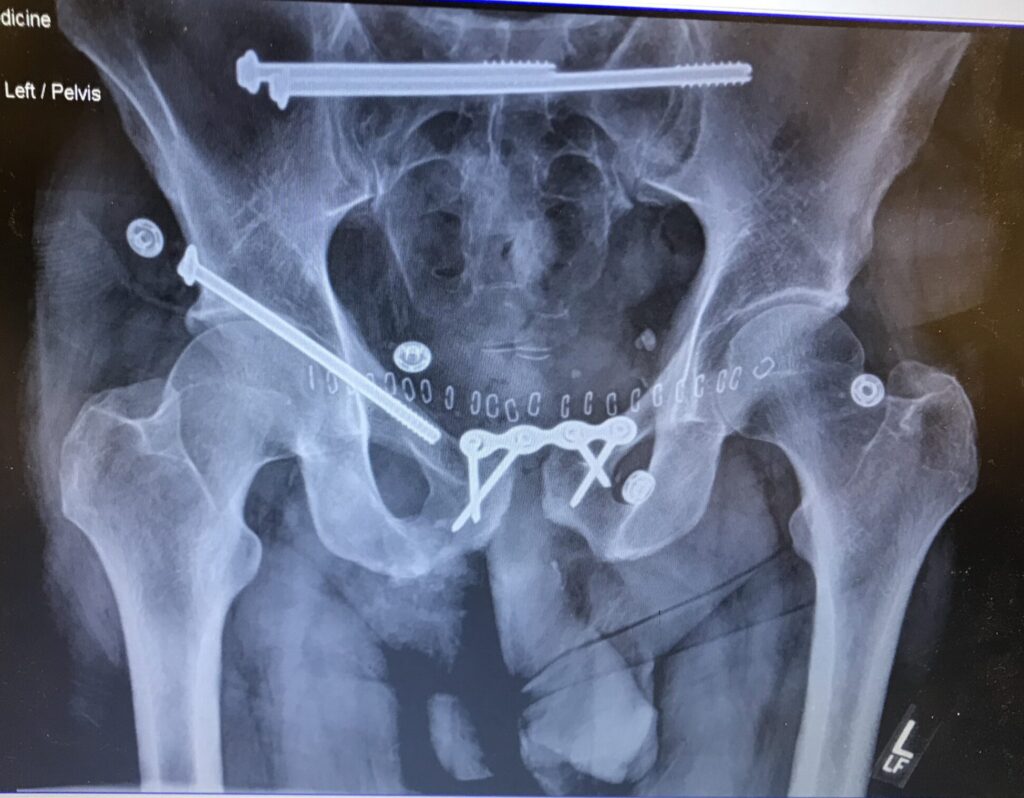
Millimeters separated Dan from death that day. His firm grip on the wheel saved him from slipping underneath the vehicle’s several-ton frame. Instead, the truck dragged his entire body, breaking his back, shoulder, pelvis and several ribs and lacerating his spleen and aorta. Had it not been for a nearby emergency vehicle, he would not have survived the internal bleeding on the way to a nearby trauma center in Portsmouth, New Hampshire.
Dan’s wife Kim, horrified by his disfigured appearance in the hospital, felt helpless. She tried wiping dirt and grass from his mouth and listened to him mumble a few words before staff wheeled him into the operating room for an emergency surgery lasting almost seven hours.
“I said goodbye to him and cried all night,” said Kim, whose own physical disabilities required the assistance of her husband at their home in Salisbury. “I couldn’t help but think it might be the last time I’d ever speak to him.”
Despite coding twice, Dan managed to survive his traumatic injuries, but not without surgeons making a harrowing discovery. Several full-body tests revealed a large mass in Dan’s neck. The mass wrapped around his wind pipe, deep beneath the surface of his skin.
“I’ll never forget the doctors asking me, ‘How had you not struggled to breathe this whole time?’” said Dan, whose body was kept together by dozens of surgical screws and plates. “The truth is, I was on a collision course with another disaster the whole time.”
His enrollment in a groundbreaking clinical trial led by Gregory W. Randolph, MD, FACS, FACE, director of the Thyroid and Parathyroid Endocrine Surgical Division at Mass Eye and Ear, would ultimately spare him from another catastrophe beyond repair.
An impossible choice
Amid his recovery from the crash, Dan was formally diagnosed with thyroid cancer, a common malignancy with a generally favorable prognosis. Surgeons regularly remove such cancers from the front of the neck using intraoperative nerve monitoring technology. The tools help surgeons avoid structures critical for breathing, speaking or swallowing, especially when removing the thyroid or parathyroid glands at the front of the throat. Surgeons then treat patients with radioactive iodine to erase any remaining, microscopic cancer cells.
Dan’s cancer proved exceptional; it was six centimeters long and so advanced that it had already invaded his trachea, larynx and the tissue over his spine. Its size afforded surgeons little space to navigate the inside of the neck, leaving Dan with two choices: Surgeons could either remove a small part of the cancer, but not all of it, or they could eradicate the entire disease by removing large parts of the invaded structures. The latter would significantly impact Dan’s voice and his ability to swallow or breathe.
“It is a difficult decision,” explained Dr. Randolph. “Removing the entire cancer could have forced him to spend the rest of his life without a voice box or eating through a feeding tube, whereas removing part of the cancer would leave behind enough of the disease for it to spread even deeper into his body.”
Dan was only 50 years old; he wasn’t ready to live the last few decades of his life mired by countless comorbidities. After all, he still needed to care for his wife. Kim was determined to exhaust all options for her husband, yet few doctors outside Boston knew how to treat cancers as invasive as Dan’s. When a friend of hers referred the couple to Dr. Randolph’s practice in Boston, she set up an appointment as early as possible.
Little did she know: Dr. Randolph had just broken ground on a new treatment option, one capable of eradicating invasive cancers without compromising a patient’s ability to speak, breathe or swallow.
Flipping convention on its head
In 2015, a study published in the New England Journal of Medicine caught Dr. Randolph’s attention. According to the study, patients with invasive thyroid cancer reported a significant decrease in the size of their cancers when treated with the drug lenvatinib after only a few months. Even those patients whose cancers had invaded organs as far away as the lungs and liver experienced their disease retreating into more controlled areas of the body.
Dr. Randolph saw an immediate use for the drug in the operating room.
“If I could get even a few millimeters of shrinkage in the neck, that could be the difference between taking out the larynx or not,” Dr. Randolph explained.
In 2022, Dr. Randolph formally launched a first-of-its-kind, multi-million dollar Phase II clinical trial at Mass Eye and Ear, Massachusetts General Hospital, MD Anderson Cancer Center and Memorial Sloan Kettering to test whether lenvatinib would improve surgical outcomes in patients with invasive thyroid cancer. Rather than beginning treatment with surgery followed by medication, Dr. Randolph and his team of investigators flipped the procedure of care. They provided patients with lenvatinib prior to surgery and hoped the disease would shrink enough for surgeons to safely remove the disease in its entirety.
After meeting with Dr. Randolph, Dan decided to enroll in the trial. Treatment began under the care of Lori Wirth, MD, medical director of the Center for Head and Neck Cancers at Massachusetts General Hospital and a co-investigator in the clinical trial. After undergoing radiation, chemotherapy and several rounds of the lenvatinib, Dr. Randolph noticed Dan’s cancer beginning to recede. To create a pocket large enough to extract the entirety of the cancer, he insisted on an additional dosage of lenvatinib. The ensuing weight loss from the therapy made it a difficult choice, but one Dan said Dr. Randolph made easy to tolerate.
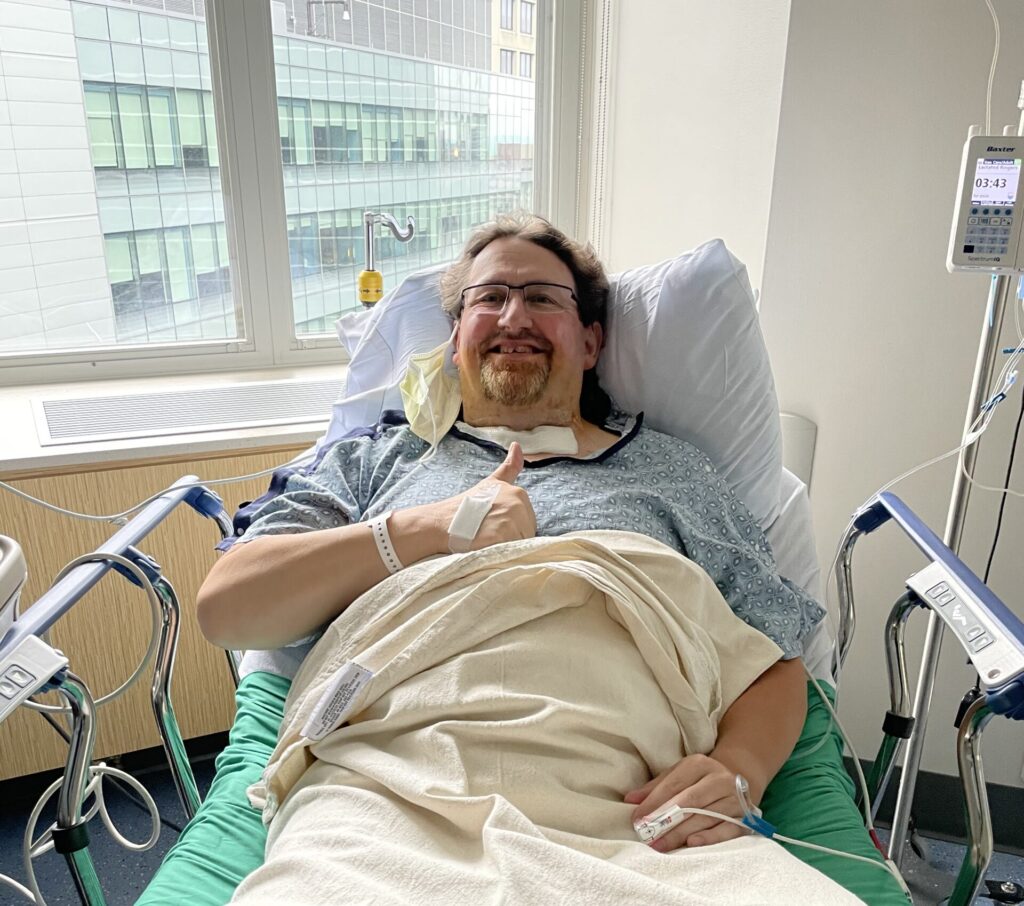
“Dr. Randolph tells it to you like it is,” said Dan, who initially felt frustrated by the loss of appetite he experienced. “He treats you like you’re human and will actually invest in what you have to say. I couldn’t see myself going against his best judgement.”
Disaster averted
Dan underwent surgery to remove his thyroid and parathyroid weeks after completing his final dosage of lenvatinib. To Dr. Randolph’s relief, the drug therapy had shrunk the cancer just enough for him to successfully remove all of Dan’s disease. Only one of his vocal cords appeared impacted, and Dr. Randolph would preserve his voice by replacing the vocal cord with a special padding.

The occasional strain Dan feels in his voices pales in comparison to the long-term effects of the truck crash. He can no long work his daily trash route and struggles to walk for long periods of time. However, he considers himself fortunate to have evaded disaster twice, and even more fortunate to call himself cancer free.
“It’s a miracle he’s alive,” said Kim. “To see him smiling, laughing and just enjoying life again is a blessing.”
Dr. Randolph credits the success of Dan’s treatment to synergy across Mass General Brigham. According to him, his collaboration with Dr. Wirth ensured he knew the exact progression of Dan’s cancer. Their constant communication and shared access to pathology reports streamlined Dan’s care to an optimal outcome, he insisted. Years ago, such information remained siloed within each discipline, often at the expense of patients, who had no choice but to sacrifice their quality of life for successful treatment.
“We’ve blended the very best medical oncology care from Mass General with the very best surgical thyroid care at Mass Eye and Ear to render complex patients more susceptible to surgery,” Dr. Randolph explained. “Now we’re on the cusp of changing what life can look like after being diagnosed with a complicated, invasive cancer. That’s synergy at its finest.”