Surgeons at Mass. Eye and Ear offer minimally invasive thyroidectomy surgeries that result in no postoperative scars.
The adverse effects of a neck scar, a de facto result of a conventional thyroidectomy, can be distressing for some patients. Thyroidectomy is currently the standard approach to removing the thyroid gland, a butterfly-shaped organ that sits in the base of the neck.
While it is very effective, the permanent scar left behind has motivated both patients and surgeons to seek alternative approaches.
Various remote-access methods to the thyroid have been developed over the years with the goal of avoiding a visible scar. The most recent and promising advancement in this arena has been the transoral approach.
A transoral thyroidectomy, which can be performed with minimally invasive endoscopic or robotic technology, accesses the thyroid gland through the lower lip. By making incisions inside of mouth instead of the neck, the procedure is completed without leaving any visible postoperative scars.
“We’ve found that the transoral approach is the ideal remote-access approach for thyroid surgery,” said Jeremy D. Richmon, MD, director of Robotic Surgery at Massachusetts Eye and Ear. “There is less flap dissection during the procedure and no postoperative scars, which makes it a good option.”
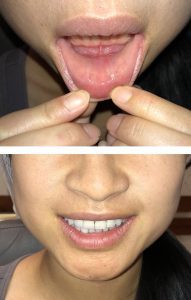
A safe and feasible alternative
Dr. Richmon has been involved in remote-access thyroid surgery since 2010. With a team at Johns Hopkins University School of Medicine, he has explored various approaches through the chest, neck, and most recently, mouth. It was his group that was the first to describe the lower lip technique in 2011.
Unlike a traditional thyroidectomy, transoral procedures start with three lower lip incisions. The distance between the lip and thyroid gland requires less tissue dissection than other remote-access approaches, making it an optimal location. After the incisions are made, laparoscopic instruments and an endoscope or surgical robot are inserted and tunneled around the jaw until the thyroid gland is reached.
Once the thyroid gland is exposed, surgery advances in a similar fashion as with traditional, open thyroidectomy, but with high-definition magnification. The critical nerves and surrounding structures are identified using this magnification and preserved as the thyroid gland is freed and ultimately removed.
Recovery is similar to that of an open thyroidectomy. Most patients are able to start on an oral diet and be discharged the same day as surgery. Risks that are unique to this procedure include lower lip swelling, bruising, and temporary numbness, which usually resolve after a few weeks.
“With the transoral approach, there is a direct pathway to the thyroid with equal access to both sides of the neck, and the magnified view is arguably better than what you can see with the naked eye,” Dr. Richmon said.
The expectation to grow
Patients with smaller nodules or cancers without lymph node involvement are the most appropriate candidates. To date, approximately 55 centers worldwide have treated patients with this approach. Surgeons do expect these numbers to grow, however, as this surgery has been determined to be safe and reproducible for select high volume endocrine centers.
“For the right person, transoral thyroidectomy is a tremendous advance that may ultimately help preserve the quality of life for our patients,” Dr. Richmon concluded.
About Our Expert
 Dr. Jeremy Richmon specializes in head and neck cancer and microvascular surgery, and is an expert in minimally invasive robotic techniques in the head and neck. Dr. Richmon sees patients at Mass. Eye and Ear, Main Campus.
Dr. Jeremy Richmon specializes in head and neck cancer and microvascular surgery, and is an expert in minimally invasive robotic techniques in the head and neck. Dr. Richmon sees patients at Mass. Eye and Ear, Main Campus.
Hi Doctor i recently was detected with thyroid cyst in which it says its solid with liquid fill in all blood tests ok except ige is 484 i was afraid to go for fnac as one of the dr said if u go for fnac it can spread if anything wrong is there so pls advice me what to do
Hi Syed, thanks for reading and your comment. We unfortunately can’t give medical advice over our blog, but if you’d like to schedule a consultation with a doctor in our thyroid division, you can call 617-573-3954, and visit here for more information.