Alopecia affects more than just a full head of hair; it can rob a person of their self-esteem and confidence. Linda N. Lee, MD, discusses the complexities of hair loss and available treatments.
Hair loss, or alopecia, can take a heavy psychological toll. Many individuals are willing to pay exorbitant amounts of money to keep their hair from falling out, which has helped fuel a multi-billion-dollar treatment industry. Each year, the industry grows larger, as do some of the claims promoted in advertisements for an array of treatments.
Focus caught up with Linda N. Lee, MD, a facial plastic and reconstructive surgeon in the Facial and Cosmetic Surgery Center at Mass Eye and Ear, who warned that patients should learn more about their hair loss before committing to any kind of treatment option.
“Hair loss can be devastating, so people can become pretty desperate in terms of wanting to try different treatments,” she said. “With all the marketing directly being fed to consumers, people need as much reliable, evidence-based information on their side as they can find.”
What is alopecia?
Alopecia can occur in several different forms. In some cases of autoimmune disease or scarring alopecia—such as alopecia areata—the body attacks its own hair follicles, causing hair loss and preventing hair from growing on the scalp. In these cases, primary treatment is often aimed at treating the underlying scarring process through medication or steroids, rather than through hair transplant surgeries.
The most common form of alopecia is androgenic, which begins as a thinning or receding of hair and progresses with age. According to the National Institutes of Health, androgenic alopecia affects nearly 50 percent of men by age 50 and more than 20 percent of women. The progression of alopecia differs by sex, too. For men, it typically begins along the temples and at the crown of the head, whereas women might experience thinning throughout the scalp and increased hair loss by menopause.
What frustrates physicians most about androgenic alopecia, Dr. Lee said, is the inability to pinpoint a single clear cause. Wives-tales often point to maternal genes as a predictor for early-stage alopecia, and some experts have suggested hormones as a possible explanation. However, neither claim has been universally accepted, nor does either account for other known factors such as weight loss, smoking, stress or even anesthesia from surgery.
Women who are pregnant, for example, might report drastically different cases of alopecia despite having pregnancy-related elevated hormone levels.
“I’ve seen women lose tons of hair at different trimesters of their pregnancy, and I’ve seen others who are amazed by how full and healthy their hair looks,” said Dr. Lee. “There really isn’t a foolproof way of determining why one person might be more prone to losing their hair than any other.”
Psychological burden
Hair is associated with beauty, health, approachability and youth across a myriad of cultures. In a day-and-age when one’s appearance is constantly broadcasted on social media and dating apps, individuals will do whatever they can to protect their image. Just as a person wears makeup to hide a pimple or fill eyebrows, patients with alopecia will undergo hair transplants and wear hair extensions or wigs. Any one of these options can produce a significant boost in self-confidence, especially among individuals with more severe cases of hair loss.
“When I see patients, many of them are tearful about their hair loss,” said Dr. Lee. “People don’t always feel comfortable talking about it with others because they’re embarrassed, or they don’t think it warrants the same attention that other medical conditions receive.”
While hair loss has been shown to cause a loss of self-esteem and confidence, Dr. Lee believes the condition cuts deeper than many physicians know. In 2022, she sought to understand the true psychosocial burden of hair loss by evaluating the health utility measurements of men and women with alopecia. Health utility is an objective way of comparing quality of life and societal significance across different medical conditions. Over the course of the study, patients with alopecia were asked how many years of life they would trade to have a full head of hair, and their responses were compared to answers for different medical conditions.
Their findings, which were published in Aesthetic Plastic Surgery Journal, suggested the true experience of patients with alopecia was much worse than people without hair loss actually perceive, particularly among women. According to the study, women with alopecia would give up nearly the same amount of years of their life to have a full head of hair as they would give up to have sight restored in one eye. The study also showed significant improvements in health utility after hair transplantation surgery.
Can alopecia be treated or prevented?
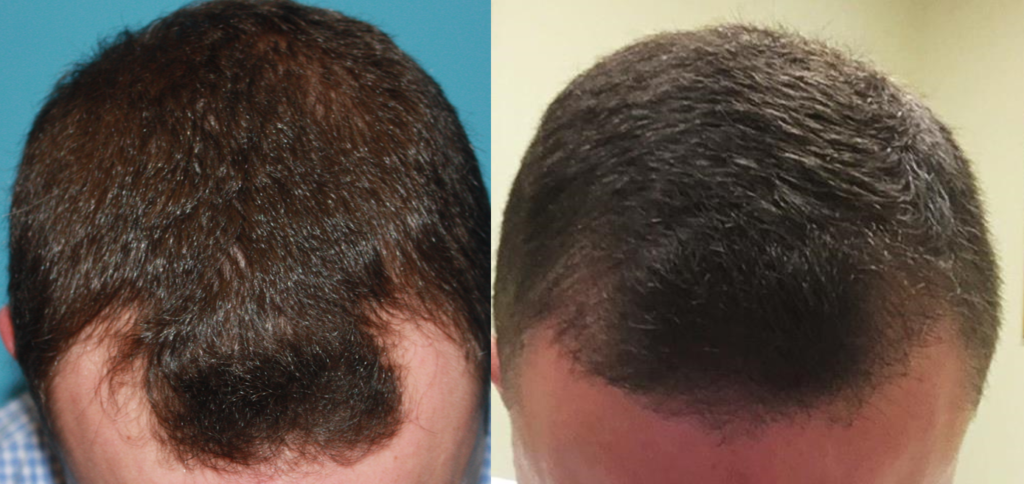
Mass Eye and Ear offers several different treatment options for patients with alopecia. One of the most popular is a hair transplant, which extracts hair follicles from a part of the scalp with strong, healthy hair and implants them onto a different area with hair loss. Decades ago, surgeons would implant follicles in “plugs,” which resulted in an unnatural or “surgical” appearance. Today, the technology has improved, and surgeons transplant single hair follicles one-by-one, providing patients with hairlines that look more natural.
The procedure typically lasts five-to-eight hours yet requires no anesthesia and leaves few signs of surgery. Results are not immediate; those who undergo a hair transplant can wait up to a year to see hair growth. Those who desire more hair density can repeat a hair transplant one year from their initial procedure. For patients looking to prevent the progression of their alopecia, Dr. Lee recommends a variety of topical foams and over-the-counter medications approved by the U.S. Food and Drug Administration (FDA) as a first-line treatment.
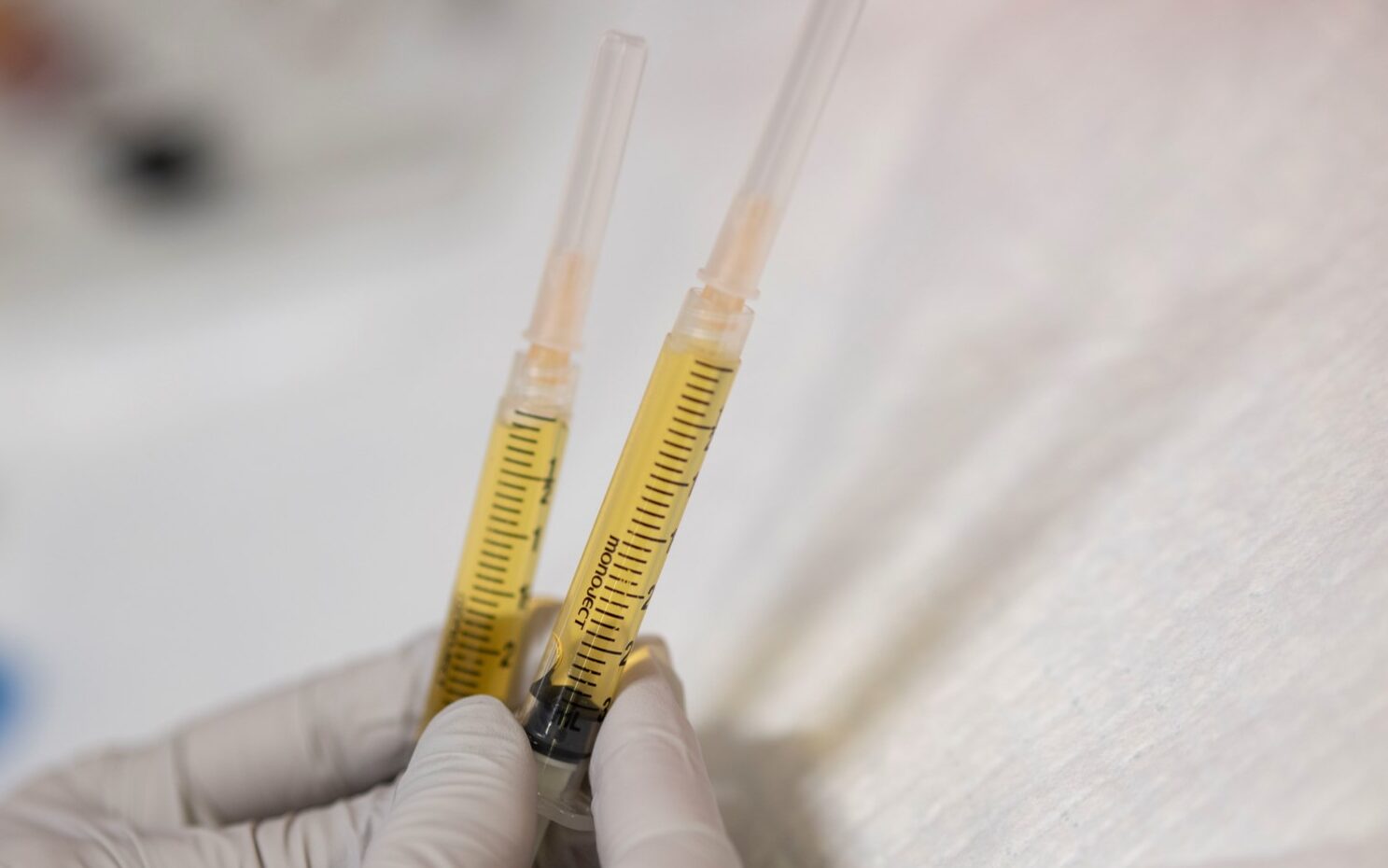
Newer options for slowing hair loss have emerged in recent years. The FDA recently approved oral minoxidil, or “oral ROGAINE®,” which is ingested instead of directly applied to skin as a foam. The medication is typically prescribed by a dermatologist or primary care physician specializing in hair loss, either of whom can help monitor any undesired changes in blood pressure that might occur from treatment. Platelet-rich plasma (PRP) injections are another relatively new treatment option. Blood drawn from a patient is centrifuged and distilled into a gold-colored serum rich with growth factors. The serum is then injected into areas of hair loss to stimulate growth and slow down shedding among remaining hair follicles.
Since no two heads of hair are exactly the same, treatments vary from person-to-person. A consultation with a board-certified specialist, Dr. Lee maintained, remains the best first step toward any solution. If hair loss is determined to be androgenic and non-scarring, a consultation with one of Mass Eye and Ear’s hair loss surgeons can help a patient determine whether they are a surgical candidate for either a hair transplant or PRP injections. Topical treatment discussions are best suited for dermatologists or primary care providers.