Few people know their body as well as Betty Doyling, a personal trainer from Warwick, Bermuda. That said, a pituitary tumor was the last thing on Betty’s mind. A collaboration between George A. Scangas, MD, a sinus and skull base surgeon at Mass Eye and Ear, and the Neuroendocrine and Pituitary Tumor Clinical Center at Massachusetts General Hospital, would prevent the tumor from ruining her eyesight.

Betty Doyling was a model of perfect health.
For years she worked as a personal trainer in Bermuda. She had never broken a bone in her body, let alone undergone any kind of major medical procedure. Her healthy diet and love for running kept her in shape and full of energy.
Needless to say, it came as a surprise when she stepped on the scale one morning and noticed a sudden change in her weight. She had gained 30 pounds in little under a month. She attributed the change to too many home-cooked meals during the pandemic. But then, out of the blue, the 43-year-old began lactating.
“I knew I wasn’t pregnant,” said Betty, a mother of two children. “I just remember thinking to myself, ‘Oh no, what’s going on?’”
After a visit to her local OBGYN and her endocrinologist, Betty underwent an MRI. The scan revealed a mass located at the center of her skull base. Further tests showed a pituitary tumor, and one that was dangerously close to her optic nerve.
“I’ve always heard stories of other people having tumors, but I never, ever thought it would be me,” Betty explained to Focus. “When my doctor told me I had a tumor, I remember thinking to myself, ‘This has to be a mistake.’”
A second opinion proved the diagnosis to be no mistake. This led her to fly hundreds of miles north to have the tumor removed by Dr. George Scangas, a sinus and skull base surgeon at Mass Eye and Ear, or risk losing her eyesight.
It kept growing, growing, growing…
According to Dr. Scangas, approximately one of every 10,000 people develops a pituitary tumor in their lifetime, making it one of the most common types of brain tumors. The pituitary gland, which is pea-sized, sits in a tight space along the skull base, right behind the nasal sinuses and between the eyes. While tiny, the gland is responsible for regulating vital hormones for growth, blood pressure and reproduction.
Most often, pituitary tumors are benign. However, they become dangerous if they grow too large and press against the optic nerve, jeopardizing a person’s vision. Upon discovering Betty’s tumor, doctors in Bermuda first attempted to shrink the tumor using medication. Eight weeks later, the tumor had not shrunk and was beginning to press against the nerve.
As a personal trainer, Betty couldn’t afford to lose her vision and her ability to focus on her clients. She also knew how debilitating poor eyesight can be from her mother, who was legally blind.
Doctors would need to extract the tumor from the middle of Betty’s head to keep her eyesight out of harm’s way. There was just one problem: Not a single doctor in Bermuda could perform the sophisticated endoscopic procedure needed for the extraction. Thankfully, her endocrinologist, Andrew Jamieson, MRCP, PhD, knew the best place to go.
“He told me that if he had this particular tumor, Mass Eye and Ear and Massachusetts General Hospital would be the only place he’d go to get treated,” Betty said. “Before I knew it, I had my flight booked and I had a date scheduled for surgery.”
Pulling a tumor out through the nose
Surgeons have little margin for error when extracting a pituitary tumor. The pituitary gland sits too close to critical structures – such as the optic nerve, major arteries and the brain – for doctors to slip by even a millimeter. One wrong move could result in impaired vision, damage to the skull base or, in extremely rare cases, uncontrolled bleeding and stroke.
So, how does a surgeon safely pull a pituitary tumor out from someone’s head? By going through the nose. In a minimally invasive procedure called a transsphenoidal anterior skull base surgery, a rhinologist uses an endoscope to open the sinus so that a neurosurgeon can extract the tumor from the skull base. After extraction, the rhinologist repairs the skull base, which keeps the brain separated from the nasal and sinus passages.
At the Mass General Neuroendocrine and Pituitary Tumor Clinical Center, Dr. Scangas and neurosurgeon Brooke Swearingen, MD perform these complex procedures on a regular basis to ensure optimal outcomes. The center provides an integrated approach to patients with pituitary and hypothalamic disorders, bringing together the expertise of more than 20 physicians specializing in neurosurgery, endocrinology, neurology and radiology at Mass General, and rhinology at Mass Eye and Ear. The expertise and familiarity between each doctor at the center are what make these complicated procedures fairly routine.
“The more you work with a specific co-surgeon, the more streamlined the process becomes, especially with a procedure as complex as anterior skull base surgery,” Dr. Scangas said. “The MGH neurosurgeons and Mass Eye and Ear rhinologists have an incredible relationship. Our experience and teamwork make a huge difference in the care of our patients and is such a strength of the Mass General Brigham system.”
Trusting the recovery
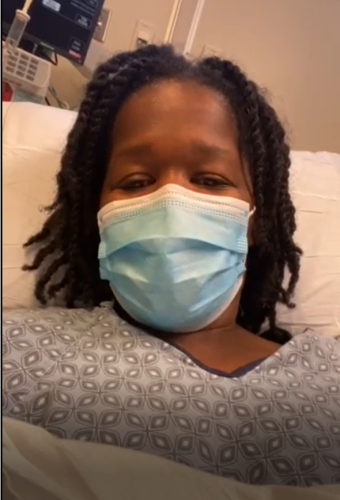
Ahead of her visit to Boston, Betty logged on to Facebook. She wanted to speak with patients who had undergone the procedure to better understand exactly how long her recovery might take. The possibility of a cerebral spinal fluid leak from a faulty skull base repair gave her the most anxiety, she said.
Dr. Scangas made sure this was never an issue. During Betty’s procedure, he repaired the skull base with fat from her abdomen and a mucosal graft from her sinus. He also advised Betty to avoid strenuous workouts for four to six weeks. Too much pressure on the newly repaired skull base, he said, could cause the graft to fail and the spinal fluid leak to return. That meant no running and no weightlifting, a lofty challenge for the personal trainer.
“The doctor-patient relationship is crucial with these surgeries,” Dr. Scangas said. “Despite the significant impact these restrictions had on her livelihood, Betty did a fantastic job of taking our recommendations seriously and putting her health and recovery first.”
A month and half after her surgery, her faith in Dr. Scangas was rewarded. She began working out with her clients in Bermuda again and felt no signs of a leak through her nose. As she picked up the intensity of her workouts, she felt at ease and back to her normal self. The model of health she once embodied was returning to plain view.
“I had talked with so many pituitary tumor patients who did not go to Mass General or see Dr. Scangas for their procedure,” Betty said. “They had run into so many nightmares in their recovery. I experienced none and am forever grateful for their care.”



Due to irregular thyroid levels, I had an MRI performed over 4 years ago at MGH. A pituitary adenoma was discovered. I was fortunate enough to have Dr. Swearingen perform the surgery to excise the small tumor. All went well. No vision problems. And my recent MRI 4 years later showed no problems and no growth. Thank you Dr. Swersingen, Dr. Kaulbach and MGH.
Dr. Scangas is the best. He removed a Schwannoma nasal from my head in 2019. I feeling great. May God bless him