A number of patients who received ventilator support while hospitalized with COVID-19 have developed issues in their airways and vocal cords that, if left untreated, can cause permanent damage.
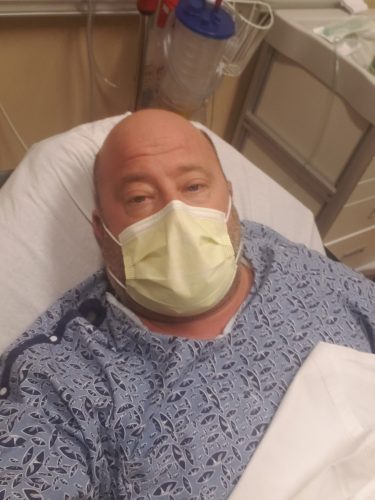
Veikko Huuskonen had already survived one of the most trying experiences of his 48 years following his hospitalization with COVID-19 in March 2020. The last thing he expected was that his life-saving care would lead to new airway problems that would require urgent medical attention.
The Hampstead, NH resident was the first person to walk into the emergency department at Holy Family Hospital in Methuen, MA and be diagnosed with COVID-19 on March 26, 2020. He drove himself there on the guidance of doctors after a low reading on his pulse oximeter and symptoms of this new disease that had only recently started making headlines worldwide. Once admitted, Veikko was placed in a medically-induced coma on a ventilator for 21 days. He fought to stay alive as his kidneys shut down. He lost 35 pounds. Thankfully, he recovered. Veikko was discharged nearly a month later, wheeled out to the sounds of thunderous applause from the hospital staff who were so grateful for his recovery.
After inpatient rehabilitation where he needed physical, occupational and speech therapy, he finally returned home in May. But soon after, he experienced difficulty breathing.

“I didn’t know what it was, and assumed it was normal allergies and congestion,” Veikko told Focus. A local ENT told him upon examination, “You have a problem here.”
Veikko was diagnosed with laryngeal and tracheal stenosis, a condition in which the throat and windpipe are abnormally narrow. Typically an adult’s airway is 15 to 25 millimeters in diameter, but Veikko’s was only 5mm, and his ability to breathe was affected.
“It was like I was breathing through a McDonald’s straw,” he said. Veikko would later learn he was not alone with this issue.
Program launched to help patients with post-COVID-19 airway problems
There have been nearly 30 million COVID-19 cases in the U.S., with many resulting in hospitalization and a percentage of those cases requiring intubation and ventilator support. Early studies suggest that approximately 20 percent of patients who have had intubation or tracheostomy after COVID-19 will develop a central airway problem, such as an abnormal laryngeal finding, including stenosis and vocal fold paralysis. If not treated early, some of these problems can be permanent.
Phillip C. Song, MD, director of the Division of Laryngology at Massachusetts Eye and Ear, had seen enough of these cases come into his clinic that he knew something had to be done on a larger scale.
“After the first surge, the number of these cases were slamming our practices,” he told Focus. “They were all similar: patients who were put on ventilators had developed airway problems that required immediate treatment, or they risked permanent damage. We had to get the word out so patients and doctors knew to be on the lookout for these problems following COVID-19 hospitalization.”
This led Dr. Song to start a new consortium of doctors across the Massachusetts area to treat and research this complication, including physicians from Mass Eye and Ear, Brigham and Women’s Hospital, Massachusetts General Hospital and Spaulding Rehabilitation Hospital – all members of Mass General Brigham.
“Because COVID-19 is a new problem that uniquely can affect patients’ central airways, we needed to utilize the expertise of multiple types of surgeons and specialists to tackle these problems effectively,” he said.

Issues related to this prolonged ventilation include: weakness and immobility of the vocal folds on the larynx that regulate airflow into the lungs, stenosis of the larynx and trachea, scarring of the airway, infections, and masses and ulcers on the vocal folds.
Dr. Song encourages COVID-19 patients to seek care immediately with an otolaryngologist if they are experiencing airway symptoms after their hospital discharge. These patients might require follow-up care from a different type of surgeon or rehabilitation doctor, depending on their case.
Interventions aimed at restoring airway function and breathing
Veikko underwent a nonsurgical procedure to widen his trachea at a local clinic. He then made his way to Mass Eye and Ear for a second opinion where he saw Dr. Song. Veikko was hesitant to undergo surgery because of all he had been through, so they decided to try some conservative approaches, including another tracheal dilation and a steroid injection. He underwent endoscopic surgery, multiple rounds of steroid injections, a laser procedure to remove some of the scar tissue around his airway, and chemotherapy to prevent the scar tissue from growing back.
At one point throughout his treatment, Veikko developed an infection. His doctors recommended that he go to the emergency room at Mass General Hospital, where he was given antibiotics. Dr. Song then told him that they had done all they could with endoscopic surgery to fix his problem, and that Veikko would benefit from a tracheal resection and reconstruction, a surgery to remove a portion of the windpipe. Dr. Song referred him to a member of the airway consortium, Michael Lanuti, MD, a thoracic surgeon at Mass General Hospital. The surgery was a success.
“After the surgery, I could finally take a solid breath,” said Veikko. “Dr. Song and Dr. Lanuti basically saved my life, and if my crazy story can help other people not delay getting their airway symptoms checked out, I’ll be happy.”

Seeking care after signs of airway problems
If a patient is experiencing any of these problems following their hospital discharge after COVID-19, they should immediately be evaluated by a laryngologist or otolaryngologist:
- Hoarseness
- Voice changes
- Cough
- Shortness of breath
- Noisy breathing
- Difficulty swallowing
- Throat pain
- Foreign body sensation
A patient with these symptoms may have to undergo an examination and airway tests, in addition to imaging, such as chest X-rays and CT scans.
“It is crucial that patients do not delay getting seen. The earlier the problem is treated, the better the outcomes are,” said Dr. Song. “We’ve seen patients who have permanent vocal cord and airway damage, and sadly, as cases continue to rise, we expect to see more people affected.”
Please call Mass Eye and Ear’s Laryngology Division at 617-573-3557 if you or someone you know is interested in being evaluated for airway complications. We are committed to the highest standards to ensure the safety and well-being of all patients, visitors and staff.


What an inspiring story!! Congratulations for following through on your medical needs.
Thanks for your kind words, Heather! We’ll pass along to Veikko.