The Mass Eye and Ear/Harvard Medical School’s Otolaryngology–Head and Neck Surgery (OHNS) Residency Program was recently selected by Residency Navigator from Doximity as the top program of 2020-2021. Focus spoke with PGY-5 chief resident Dr. Shekhar K. Gadkaree and PGY-3 resident Dr. Ciersten A. Burks, to hear about their experience in the program first-hand, and what incoming residents might expect. Read a Q+A with the residency program’s directors.
What made you choose this residency program?

Dr. Gadkaree: I wanted to join a residency program that offered a deep and comprehensive experience in all areas of Otolaryngology–Head and Neck Surgery (OHNS). Having good mentors was important to me, but the ability to get exposure to a wide array of specialties was just as important.
Arguably, my number one priority, however, was a residency program with a good culture. I had a friend from medical school who was a resident at Mass Eye and Ear whose point of view was invaluable. Ultimately, I chose Mass Eye and Ear/Harvard Medical School because I knew I’d receive top-level, in-depth training and be part of a culture that helps you thrive educationally and personally.
Dr. Burks: There are so many things that drew me to this residency program. While interviewing here, I learned more about the wide breadth and depth of surgical training and research opportunities in each of the subspecialties of otolaryngology. However, it was honestly the people who made me want to come Mass Eye and Ear/Harvard Medical School. The people here create a culture that thrives upon mentorship and support. At the residency dinner the night before the interview, I saw firsthand how close-knit the residents were and how they were genuinely excited to see one another. From that moment, I could see myself being part of this group.
How has working at a dedicated specialty hospital for OHNS helped your training?

Dr. Burks: There are so many advantages of being at a unique OHNS specialty hospital like Mass Eye and Ear. For one, in addition to the surgical and clinical expertise that is gained from working with our attendings, we are surrounded by experts from various fields who are dedicated to OHNS patient care. From the nursing staff to surgical technicians, speech and language pathologists to radiologists and anesthesiologists – there is so much to be gained from the wealth of knowledge around us that is focused on the management of patients with otolaryngologic conditions. Additionally, we have our own emergency department (ED) dedicated to the care of patients presenting with OHNS concerns. The learning experience in the ED has been one of the most valuable during my residency training thus far. All of those components make Mass Eye and Ear extremely unique and have been paramount in shaping my training.
(Watch the video above to take a virtual tour of our residency program.)
What is some of the research you participate in?
Dr. Gadkaree: One of the best things about being at a specialty hospital with an OHNS focus is that we’re afforded the opportunity to work closely with experts who are doing research in a variety of different fields. It’s so beneficial to have research integrated as part of the experience.
In my time here, I have gotten pulled into a diverse array of research projects. I have a bioengineering background and sometimes work on engineering-related projects, but I was also interested in public health and refugee health care, and was able to foster that interest. One of the main things I’m looking at is socioeconomic barriers and access to care and how physician and patient decision-making lead to varying patient outcomes. As an example, we are currently looking at provider distribution – if you have a lot of subspecialty surgeons in one area, do people have more/better outcomes? And how does medical insurance impact outcomes and patient decision-making at these hospitals?
Many of the residents conduct diverse research, and some choose an extra two-year research track. We’ve had residents interested in health care utilization and how to optimize operating room times to provide the best care. Some are interested in clinical trials. Several do basic science research, including research on the auditory brainstem and facial nerve reanimation.
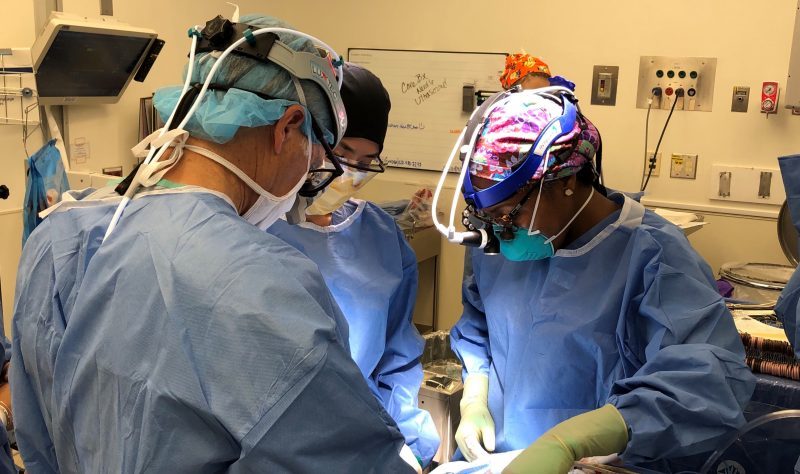
Dr. Burks: We are fortunate to have many different resources and collaborators available within Mass Eye and Ear and the Harvard Medical School network. My research has focused on addressing health care disparities and diversity in the surgical workforce. I have worked closely with the Brigham and Women’s Center for Surgery and Public Health which holds the mission of advancing surgical research to inform policy and the development of programs for equitable patient care. It has been a tremendous experience and I am so thankful for mentors there and within Mass Eye Ear to further my research endeavors.
How has COVID-19 impacted your education?
Dr. Gadkaree: When COVID-19 first started, we were extremely busy with our typical surgeries and clinical responsibilities. Gradually, the pandemic moved from the background into the forefront of our clinical experience every day. Even though elective surgeries were cancelled, many head and neck cancer cases were still happening, so there was still plenty of OHNS activity during this time. We had to split into skeleton crews to limit exposure to other residents.
As residents, we were eager to figure out how to help in the response to the pandemic. Many people in our program volunteered to be redeployed to other hospitals and units, and many of our nurses were redeployed to other hospitals. Once Mass Eye and Ear converted one of its floors into a COVID-19 rehabilitation unit, our entire program volunteered to help take care of COVID-19 positive patients in this capacity.
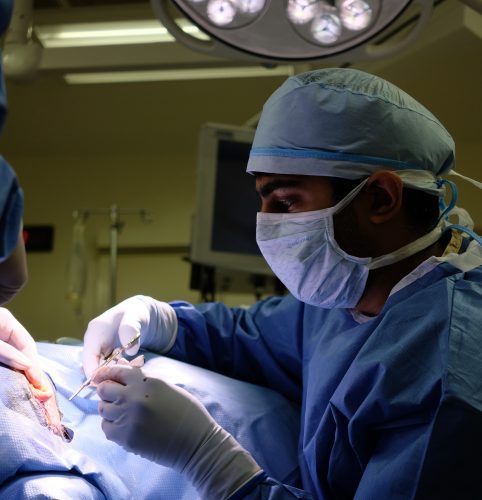
During the period when elective surgeries were cancelled, we were also faced with more time to think about research projects and what questions may be worthwhile to explore in the face of the COVID-19 pandemic. One of my Facial Plastic Surgery attendings and I went to the cadaver lab and started a project looking at aerosolization in facial plastic trauma procedures, and we also did a project around jaw surgery as well. Before we got directly involved in the response, we made the most of our time to continue our education through creative avenues including research projects and online didactic sessions.
What is one thing you’d want a prospective resident to know?
Dr. Gadkaree: We are a family and everyone truly gets along with one another; we go hiking on weekends, see each other after work, play sports together, and go out for runs or for socially-distanced drinks. The residents here are my best friends. You join a family where everyone supports one another, and many residents even come back as attendings. As a senior resident who’s seen the program change over time, coming to work every day is fun and something I look forward to.
Dr. Burks: While the training here is unparalleled, it is truly the family at Mass Eye and Ear/Harvard Medical School that has made this experience such a special one. It has been an honor to train alongside such an inspiring, compassionate and hard-working group of co-residents. I learn from them, share triumphs and disappointments with them, and have felt so supported by them. I am so thankful for this place and the lifelong friendships that have started here. It is the best group to be a part of and we look forward to meeting those who will join us!
What are your future plans beyond residency?
Dr. Gadkaree: Once I leave residency in June 2021, I will be joining the University of Minnesota Medical School to begin a fellowship in Facial Plastic and Reconstructive Surgery. I had wanted to join a reconstructive surgery program that offered the full breadth of training in facial plastic surgery, so I am thrilled with the opportunity to continue my training there.
Dr. Burks: As a PGY3, my future plans are not yet set; however I am certain that this program will prepare me well with phenomenal clinical/surgical skills and mentors – no matter what I decide to pursue.


The MEEI Head and Neck Surgery Residents are extremely lucky to be able to learn from Derrick T. Lin, M.D., the best in the business!!!
Thanks so much for this wonderful comment, David. We agree!