In the past decade, 16 residents from the Mass Eye and Ear/Harvard Medical School Otolaryngology–Head and Neck Surgery (OHNS) Combined Residency Program have been awarded prestigious Centralized Otolaryngology Research Effort (CORE) grants by the American Academy of Otolaryngology–Head and Neck Surgery Foundation (AAO-HNSF). This past June, Roy Xiao, MD, a PGY-3 resident, became the latest resident to receive the grant.

Two pillars central to Mass Eye and Ear’s vision are conducting cutting-edge research and teaching tomorrow’s medical leaders. The Otolaryngology–Head and Neck Surgery (OHNS) Combined Residency Program has done an exceptional job of accomplishing both. After all, five months of residency are dedicated to research in a resident’s PGY-3 and PGY-4 years.
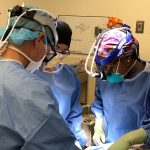
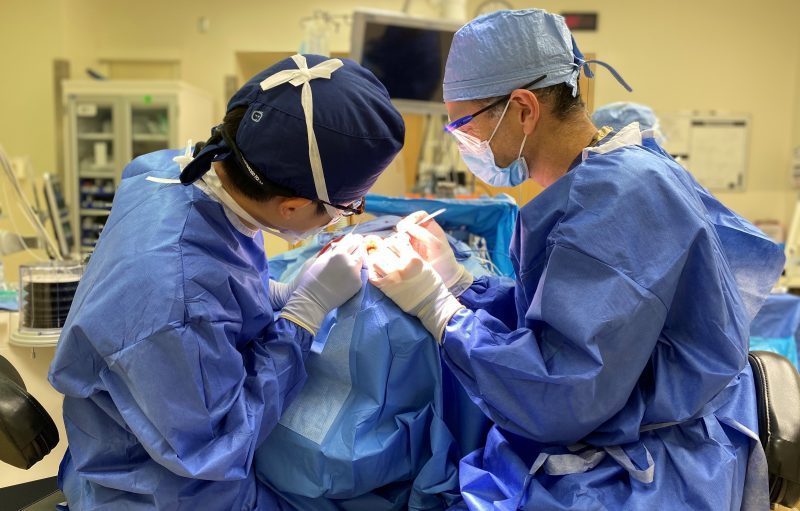
Focus caught up with Dr. Xiao, a PGY-3 resident in the program who is based inside the Berthiaume Surgical Photonics and Engineering Laboratory, to learn more about his recent CORE grant, his facial plastics and reconstructive surgery research, and his mentors and colleagues who helped prepare him for this award.
Why did you decide to apply for a CORE grant?
Before I began my residency, I told Stacey Gray, MD, director of the OHNS Combined Residency Program, that a goal of mine had always been to secure funding for research by the time I graduated. I wanted a CORE grant in particular. Each year, the AAO-HNSF offers CORE grants as a way to support residents hoping to secure funding for research.
During my PGY-2 year, I knew applying for the CORE grant was an opportunity I couldn’t afford to miss out on. I had plenty of expertise at my disposal. So many past recipients of the grant attended the Residency Program and were willing to meet and lend their advice. Fellow residents Alan Workman, MD, and Shekhar Gadkaree, MD, both of whom had received the grant in 2020, provided me with plenty of guidance throughout the process, as did countless other residents and faculty.
What are you hoping to accomplish through your CORE grant research?
My research is going to focus on motor end-to-side neurorrhaphy (ETSN), which is a common procedure used to restore facial movement.
Nerves can be connected either one of two ways: by joining the ends together, or by attaching the side of one with the end of another. The latter method, which is known as ETSN, is often performed on patients with peripheral motor nerve deficits, such as facial palsy, and helps support motor function. If a facial nerve isn’t working as it should, but there’s an established neural pathway in its place, you can supercharge the nerve by connecting the end of a donor nerve to its side.
While ETSN has been proven to restore muscle movements, doctors still don’t understand the method’s underlying mechanism. My proposed research will attempt to distinctly label and visualize regenerating axons in exquisite detail. This would allow us to understand how nerves connected in end-to-side fashion interact and yield muscle contractions. Our hope is to fill the knowledge gaps that remain from this procedure, which could lead to substantive changes in microsurgical nerve repair. This will continue to advance the lab’s work that has been made possible by generous donations from the Berthiaume Family.
How did you learn how to write a grant?
David Jung, MD, PhD, director of the Joseph B. Nadol, Jr. Surgical Training Laboratory at Mass Eye and Ear, leads the residency program’s research curriculum. He also teaches our Issues in Research course for PGY-2 residents, where we are advised to write a grant by the end of his course. This was the first time I had ever written a grant. It was a completely different experience from the abstracts and papers I was used to writing.
The biggest difference was in the clarity of language I had to use. I needed to condense five, six, seven pages of a complex topic, such as nerve reinnervation, into a few paragraphs that clearly explained why the topic is important enough for research, and then articulate how I would use the funds to conduct it.
How did you choose your research focus?
Nate Jowett, MD, PhD, facial plastic and reconstructive surgeon at Mass Eye and Ear, first proposed the idea of studying end-to-side neurorrhaphy using techniques developed over the past three years inside the Berthiaume Laboratory.
I reviewed many prior successful proposals from the lab, including those from past CORE grant recipients and current chief residents Suresh Mohan, MD, and Adeeb Derakhshan, MD. I wanted to understand how they developed and presented their research questions. I then met with lab members almost daily for several weeks to talk about grants and their own past experiences applying for them. Dr. Jowett and the entire laboratory really helped me refine my writing.
Where does your interest in facial nerve surgery come from?
I honestly didn’t know a whole lot about facial nerve surgery before I joined the residency program. My facial plastics rotation during my PGY-2 year was when I first had the opportunity to work with Dr. Jowett and Tessa Hadlock, MD, director of the Facial Plastics and Reconstructive Surgery Division at Mass Eye and Ear, in the operating room.
Working alongside them both, I immediately saw the impact they had on their patients. I noticed that patients wanted to laugh and smile in a way that simply didn’t make them stick out. They wanted to feel comfortable in their own skin. To have one of these patients say, ‘You gave me back something I never knew I could have again’ when referring to their repaired smile, gave me a newfound appreciation for the specialty.
What are your plans for after residency?
Right now, I’m here to learn and grow into the best otolaryngologist possible. When I think about my future, I know that I want a strong research component in whatever career I pursue.
I have a deep appreciation for facial plastics and reconstructive surgery. There are so many different types of practices within the specialty. Whether its reconstructive, functional or cosmetic efforts, facial plastics offers such a wide spectrum of good that you can do for patients.
Learn more about the Harvard OHNS Combined Residency Program and the countless research opportunities afforded to its residents.