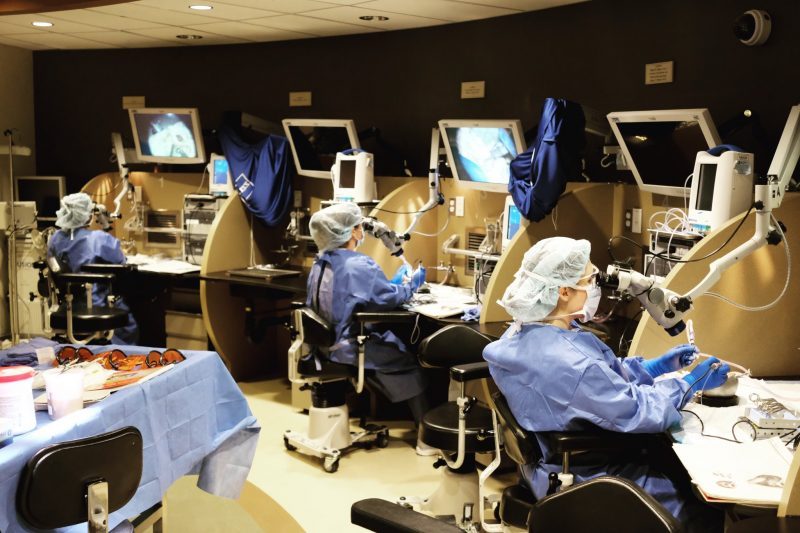
Mass Eye and Ear/Harvard Medical School’s Otolaryngology–Head and Neck Surgery (OHNS) Residency Program was recently selected by Residency Navigator from Doximity as the top program of 2020-2021, in a survey of 100,000 physicians. Focus asked Dr. Stacey T. Gray, residency program director and Dr. Kevin S. Emerick, associate program director, to discuss the program and what makes it unique. Read here for Q+A with two residents.

What makes this residency program unique?
Dr. Emerick: One of our program’s defining characteristics is that we truly are a family here. The residents are extremely close and the faculty become very close with the residents professionally and personally. It’s hard for someone on the outside of our program to appreciate the relationships formed by the faculty and residents. There is a lot of hard work in our program, but that should not overshadow the importance of the special bond that’s created between so many of the faculty and residents. I’ve seen this year after year — our family continues to grow as residents graduate from our program.
What type of applicants does our program hope to attract?
Dr. Gray: One of the wonderful things about OHNS as a specialty is that we always attract incredibly bright, passionate young physicians. We are extremely excited to train a diverse group of dedicated, hard-working and empathetic surgeons. The people who end up enjoying training here appreciate collaborative teamwork and truly value working with their resident and faculty colleagues. They are dedicated and driven to learn every aspect of OHNS and immerse themselves in all facets of training.
Dr. Emerick: We’re looking for resident applicants who really want to be difference-makers in whatever aspect of otolaryngology they end up pursuing. We want people who come from different backgrounds in terms of their personal and educational experiences. Having applicants from diverse walks of life come together will help us learn as program leaders and educators, and make the program better.
(Watch the video above to take a virtual tour of our residency program.)
What kind of research comes out of the OHNS resident program?
Dr. Gray: Research can vary from basic science bench work, to health care disparities, to medical education and outcomes-based research. One of the exciting aspects of our program is research runs the gamut, and our residents can tap into the varied expertise within our department and Harvard Medical School. We encourage creativity and we want our residents engaged in the research they are passionate about pursuing independently.
Some recent examples include: Medical ethics of palliative surgery; head and neck tumor cell analysis with single cell sequencing; identifying biomarkers for chronic rhinosinusitis; investigating new therapeutics for vestibular schwannomas; identifying modifiable risk factors for hearing loss – those are just a few. The diversity of the research is indicative of the breadth of the expertise here that residents can learn from.
Dr. Emerick: We’ve been really successful at hitting a spectrum of different types of research. Several residents doing the two-year research program have produced pretty amazing basic science work that has been published in top journals like Cell. We also have residents who have focused on exploratory research in clinical medicine as well as epidemiological studies. This includes everything from trying to better understand our surgical interventions, to healthcare disparities, to resident education.
We try to nurture whatever their interest may be. Our residents are putting out a lot of great research but that’s only one part of it; we’re also helping residents do research that they didn’t have any experience in, to improve their knowledge and skills in those areas. This will help make them well-rounded physicians and scientists.
Where do the residents head after graduating?
Dr. Emerick: We are really proud of the paths our residents have chosen over the years. They have found different tracks in academic medicine and community organizations. We’re also really proud of the fact that we don’t just produce one type of resident, but our program tends to take residents and support their strengths and follow them throughout their careers.
A major focus of our program is to provide our residents with some of the intangibles needed to lead in whatever field they choose. For example, we provide training in leadership development, becoming a strong presenter, and developing the fundamentals to become a good educator one day.
Dr. Gray: We are inordinately proud of all of our graduates, and they remain part of a large extended family that extends across the world after completion of training. Whether they choose to pursue fellowship training and academic practice, as many of our trainees do, or practice comprehensive otolaryngology in a community setting, we are excited to see how they will lead in their chosen environment.
How has the program adapted to the COVID-19 pandemic?
Dr. Emerick: COVID-19 helped us remind the residents that they’re doctors first, not just otolaryngologists, and part of a bigger medical community, and to think of taking care of patients in different ways. This wasn’t just about OHNS education, it was about being a good doctor. That was an amazing to witness; trying times forced our residents to become closer through shared experiences. COVID has been a formative experience for them all on numerous levels.
Dr. Gray: Our residents responded to the greater healthcare needs of the pandemic with grace and resilience. Many of our residents functioned as physicians outside of the field of otolaryngology, serving within different clinical hospital sites, as well as on the 10th floor of Mass Eye and Ear, which served as an acute rehabilitation unit for patients recovering from COVID-19. As a program, we were focused on making sure everyone felt safe and supported in these new roles, and our residents found this work extremely rewarding. I could not be more proud of their commitment to patient care during this extremely trying time. I believe all of these experiences will ultimately give our residents a broader appreciation for the practice of medicine. As a program, it has made us focus on what is truly important in the training of future physicians.
I am deeply impressed. Congratulations on the outstanding work you are doing!
Thanks for reading and your great comment, Dr. de Souza! We’ll be sure to pass along to the program’s directors.